Myasthenia Gravis
Myasthenia Gravis (MG) is a neuromuscular disease that causes skeletal muscle weakness, which is your body's muscles for movement. Myasthenia Gravis occurs when communication between nerve cells and muscles is impaired. This disruption prevents significant muscle contractions and causes muscle weakness.
What Are the Symptoms of Myasthenia Gravis?
The main symptom of MG is weakness in the voluntary skeletal muscles, the muscles under your control. The inability of the muscles to contract occurs because they cannot respond to nerve impulses. If the impulse is not transmitted correctly, the communication between the nerve and the muscle is blocked, and weakness ensues.
The weakness associated with MG usually gets worse with more activity and improves with rest. Myasthenia Gravis symptoms may include:
- Difficulty in communicating
- Problems like climbing stairs or lifting objects
- Facial paralysis
- Difficulty breathing due to muscle weakness
- Difficulty swallowing or chewing
- Tiredness
- Muffled voice
- Drooping eyelids
- Double vision
Not everyone has every symptom of the disease. Still, the common problem is that the degree of muscle weakness gets worse from day to day. If left untreated, the severity of symptoms typically increases over time.
Autoantibodies are formed against the postsynaptic nicotinic acetylcholine receptors in the striated muscles of MG patients. Antiacetylcholinesterase receptor (AntiAchR) antibodies destroy the postsynaptic membrane through complements. Anti-MuSK (antibody to muscle-specific tyrosine kinase) antibodies are present in some patients. Thymoma is detected in 10% of myasthenics, and thymic hyperplasia is detected in up to 70%, and most patients benefit from thymectomy. Harmful T cells that respond to the antigens in the thymus are destroyed, and myoid cells carrying AchR are typical on the thymus surface.
Note 1: AntiAchR and anti-MuSK levels are essential in MG patients.
Diagnostic Steps of Myasthenia Gravis
- History: The presence of complaints increases with activity and spontaneous remissions
- Improvement in muscle strength with acetylcholine esterase (Edrophonium test)
- Repetitive nerve stimulation test: Action potentials are recorded by giving three impulses per second to the nerve. A decrease of more than 15% in response is considered positive.
- Single fiber EMG
5.Blood test for antibodies associated with Myasthenia Gravis(MG)
- AntiAchR; It is specific for MG. It is 85% positive in generalized disease and less than 50% in ocular myasthenia.
- Anti-MuSK
- Radiological diagnosis using CT scans or MRI to rule out a tumor. Contrasted Thorax CT can trigger MG crisis.
Treatments in Myasthenia Gravis
- Anticholinesterase Agents: Pyridostigmine (Mestinon) is the most commonly used drug. Its effect starts in 30 minutes and reaches the maximum level in 2 hours.
- Immunosuppressive Treatment:Corticosteroids: Prednisone is often preferred. At the beginning of the treatment, it should be known that it may exacerbate myasthenic complaints in the first weeks, the dose should be increased gradually, and moderate-severe generalized patients should be hospitalized. Healing begins within weeks, and the dose is decreased when the desired level is reached within months.
Azathioprine (Imuran): It is used in patients who cannot take steroids, are unresponsive to steroids, and steroid dose reduction.
Cyclosporine (Sandimmune): Nephrotoxicity and hypertension side effects should be considered.
- Short-Term Immunotherapies Plasmapheresis and Intravenous Immunoglobulin (IVIg): It is used in situations that require rapid recoveries, such as preparation for a myasthenic crisis or thymectomy operation. It is given before surgery in advanced MG patients.
- Surgery: Thymectomy
Thymectomy is a recommended treatment modality that increases the chance of remission in patients with non-thymomatous autoimmune Myasthenia Gravis.
In patients who underwent thymectomy, the rate of drug-free remission was 2.1 times, and the reduction in myasthenic symptoms was 1.7 times more than in the group that received medical treatment. After thymectomy, 25% complete remission, 39% asymptomatic disease, and 70% recovery were observed in MG patients.
In closed surgeries, an average of 50% success is expected. We prefer thymectomy with a minimally invasive method, namely VATS/ROBOTIC surgery.
RATS /Robotic/ Videothoracoscopic /VATS/ Thymectomy
- Videothoracoscopic /VATS Thymectomy; is the most preferred method. It is made by the closed method by entering through two or three incisions. We remove the thymus gland through small incisions without cutting the sternum. It has many advantages, including aesthetics, less pain, and early discharge.


Figure 1: Videothoracoscopic and robotic thymectomy surgeries from our clinic.
Although thymothymectomy was an open (Median sternotomy/Thoracotomy) procedure in the past, it can be safely performed today with minimally invasive methods such as ROBOTIC and VATS. In the minimally invasive approach, the right-hand approach is often preferred.
- ROBOTIC Surgery; It has the same tiny incisions and similar indications as VATS. Generally, three ports (2 arms, one camera) are sufficient for RATS Thymectomy. The surgeon operates with small fractions with the da Vinci Robotic Surgery system. A surgeon standing at the patient's bedside during the operation helps the surgeon at the console. The surgeon operates on a 3D image, and cameras enlarge the operation area 10-12 times. These tooltips can rotate 540 degrees around their axis and mimic the wrist movements of the human hand.
In recent years, the RATS/VATS technique has been modified (classical three ports to 2 ports, bilateral approach, subxiphoid approach), such as subxiphoid RATS/VATS thymectomy and combined subxiphoid-transcervical VATS thymectomy.

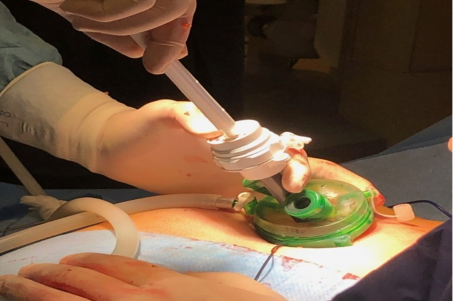
Figure 2. Subxiphoid Robotic Thymectomy
The patient is discharged between 2 and 4 days after the operation.
Frequently Asked Questions About Myasthenia Gravis
Many people have questions about myasthenia gravis. We have compiled some of the questions about this disease in detail for you, here are the questions that many people are wondering about:
In general, MG is not an inherited disease. However, it may be transmitted if a family member has an autoimmune disease. A mother can pass a temporary form of MG to her newborn child. Rarely the disease occurs in more than one family member.
Myasthenia Gravis can be treated with medications, surgery, and other treatments, alone or in combination. Treatment decisions depend on the severity of the muscle-affected disease, age, and other related medical issues.
The following factors can temporarily make your MG symptoms worse: stress, lack of sleep, illness, overexertion, pain, extreme heat or cold (outdoor temperatures, hot showers or baths, saunas, hot tubs, hot food or drinks), and certain chemicals may worsen it.
You should avoid medications that worsen MG symptoms, including certain antibiotics, beta-blockers, calcium blockers, muscle relaxants, and magnesium. Consult your primary MG doctor before taking any new medication, including over-the-counter medicines.
Yes, but your ability to work depends on the severity of your MG and your job requirements. If your MG is active, you may need to talk to your boss to see if you can temporarily adjust your workload, activities, or hours. Some myasthenia patients apply for and receive Social Security disability payments.
Exercise within your limits is highly recommended if possible. Do not exercise if you feel weak. Short sessions are tolerated more than long sessions. Start slowly using a walking or elliptical machine. When you feel tired, stop and rest. Reducing muscle fatigue is essential, and this point will vary from person to person depending on age, overall fitness level, MG symptoms, and other factors. Because your symptoms can change daily, you must talk to your doctor about how and when to exercise. Together you can create guidelines on how much exercise is healthy for you and under what conditions you should try.
If you're a woman with MG, discussing your pregnancy plans with your neurologist is crucial so you can work as a team for the best results. Together you can examine whether the pregnancy is an option, medications that need to be changed, and the risks to the fetus and newborn.
Treatment for MG involves self-care:
- Getting plenty of sleep,
- Resting your body and eyes throughout the day,
- Speeding up your activities.
It also includes good nutrition, stress management, and exercise. Myasthenia patients, like everyone else, should eat a healthy diet and maintain a healthy weight. Extra weight makes it harder to get around and aggravates other illnesses. Even if drugs like prednisone can increase your appetite, focusing on a healthy diet with plenty of fruit, vegetables, whole grains, and reasonable portions is essential. Avoid magnesium supplements unless prescribed and monitored by your doctor, as magnesium can worsen MG symptoms. Consult your neurologist before taking any supplements or alternative medications, including over-the-counter medicines, as they can affect your MG and interact poorly with other drugs.
Many myasthenia patients decide to wear medical alert jewelry, such as bracelets or necklaces. It's essential to carry a medication card in your wallet and clearly state your "Myasthenia Gravis" disease and ensure it includes your name, date of birth, phone number of a family member, your MG doctor, and any medical conditions.

