Some diseases can present themselves with various health problems, as well as cosmetical. Pectus excavatum is one of the most common diseases. The discomfort, called chest wall deformity, is usually congenital but may also occur due to other causes. So what is pectus excavatum, and what are its symptoms? Does it cause serious health problems in the future, and can it be treated? In this article, we tried to answer all the questions.
What Is Pectus Excavatum?
Pectus Excavatum, commonly known as shoemaker's chest or collapsed chest, is a chest wall deformity that occurs at birth. It refers to the collapse of the bone known as the sternum located in the front wall of the chest.
In this condition, there is an abnormal growth in the cartilage part of the ribs. With the excessive growth of the cartilage structures, the sternum collapses back.
Although genetic transmission is not shown, approximately 40 percent of patients with shoemaker's chest have a family history. Although this disease is in one in 300 to 400 births, the incidence in men is four times higher than in women. 85% of pectus excavatum patients get diagnosed within one year after birth.
It can cause asymmetry in the chest wall when it is accompanied by a disease called pigeon chest and looks like a shoemaker's chest. The effects of Pectus Excavatum disease can be physically and psychologically damaging.
Therefore treatment is inevitable.
Symptoms of Pectus Excavatum Disease and its Effects
A shoemaker's chest can manifest itself with physical and cosmetic restrictions. The most common physical symptoms are respiratory problems due to the pressure on the lungs and heart. Concomitant chest pain and shortness of breath may develop. If there is cardiac pressure, then heart rhythm disturbance may also occur.
The heart may be located in the left chest cavity in severe cases. If the disease starts to give symptoms in childhood, fatigue and shortness of breath may occur while playing games with physical activity.
The adverse effects of Pectus Excavatum disease on health are quite low. However, on the one hand, it is helpful to follow the symptoms and see a doctor and have the necessary examinations done. The complications that may present are as follows:
- When the collapse of the sternum pressurizes the right ventricle of the heart, it leads to less blood transmission to the lungs with each beat. Thus, the heart has to work harder than usual. However, it disappears entirely with the treatment of the chest wall.
- Chest wall collapse can cause self-confidence problems, especially for primary and secondary school children. This situation can cause disconnection from social life in children.
Eliminating all these effects is possible with the correction of the chest wall. Today, there is a treatment method for chest wall correction.

How Is Pectus Excavatum Treated?
There is no treatment method other than surgery. Today, there are two types of surgery methods for this disease.
The first is open surgery, also called the modified Ravitch technique, and the other is closed surgery, called Nuss surgery. Details and their advantages are as follows:
- Open Surgery (Modified Ravitch): A big incision is made in the chest wall, horizontally and vertically. The muscles under the breast tissue are retracted. We remove the cartilage structures of the ribs on both sides of the sternum; we correct the sternum. If necessary, metal plates can also be placed on the sternum.
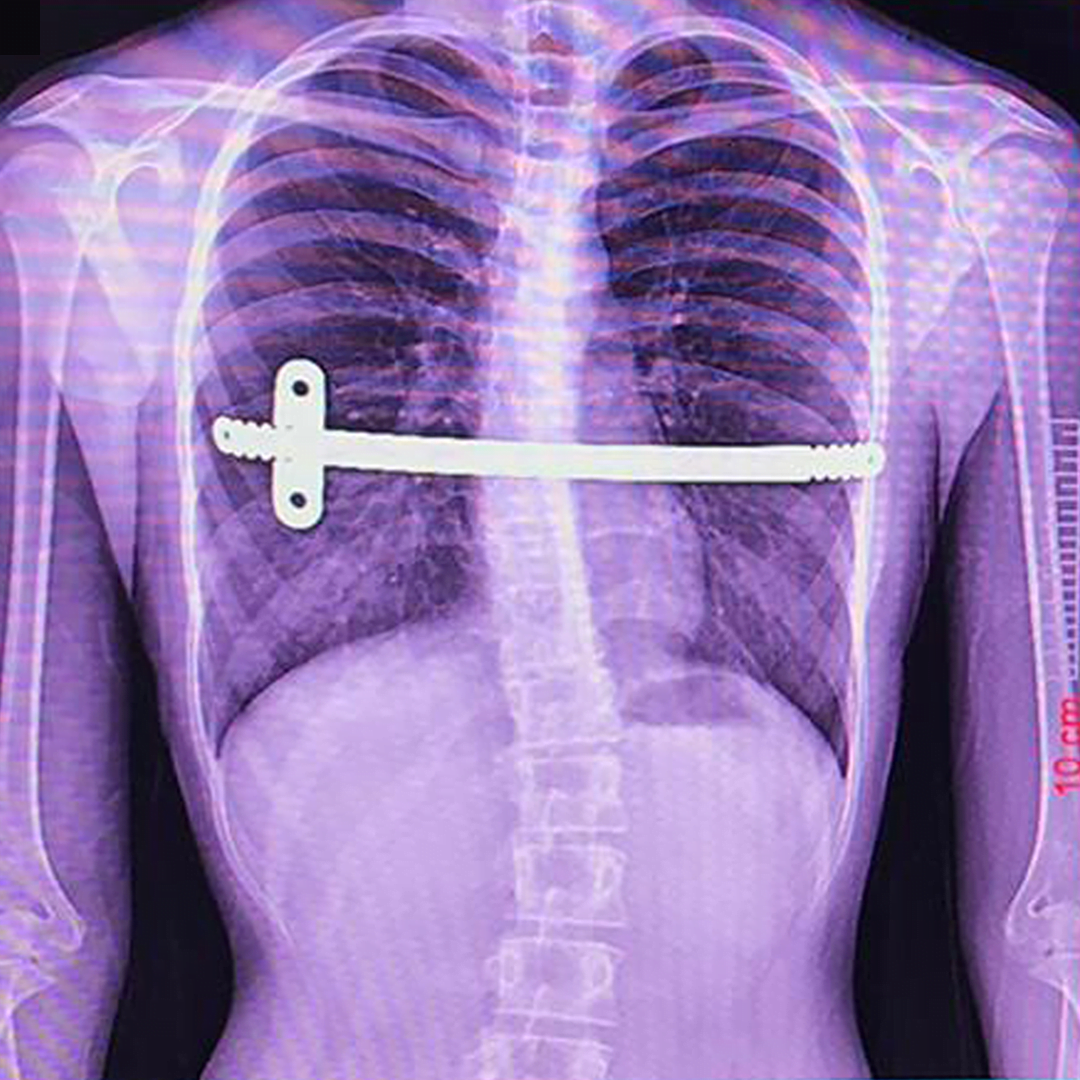
- Closed Surgery (Nuss Surgery): Small incisions are made from both parts of the chest wall. After placing it on a steel plate called the Lorenz bar, we put it in the posterior wall of the sternum. The entire procedure is performed with a camera system called thoracoscopy.
- Open surgery takes much longer than closed surgery.
- There is a much larger scar in open surgery than in closed surgery.
- Narrowing of the rib cage occurs very rarely in closed surgery; this risk is higher in open surgery and may cause respiratory problems.
- We remove the bar after two years, meaning the patient must be operated on again.
The advantages and disadvantages of these operations are as follows:
If the correct physician is selected, the probability of completing this procedure smoothly and successfully is 100 percent. Therefore, working with a specialist and experienced physician in the field is very important.

