Pleural effusion is a severe problem resulting from fluid accumulation in the patient's pleural cavity. The pleura (lung membrane) consists of 2 membranes that cover the lung and chest cavities.
The fluid accumulation in the space between these membranes surrounding the lung's outer surface and the chest wall's inner surface is called pleural effusion.
Typically, there is very little (20 ml) fluid between these two membranes. Because of many pulmonary or extrapulmonary diseases, the fluid between the membranes increases due to increased secretion and decreased reabsorption. In such cases, a condition called pleural effusion (pleurisy) occurs.
It can cause various conditions, including increased permeability of the pleural membrane, pulmonary capillary, negative intrapleural and oncotic pressure reduction, and obstruction of lymphatic flow.
Although pleural diseases constitute 1/4 of the patients hospitalized in thoracic surgery clinics, they address many risky disorders.
It is a group of diseases studied, and thoracic surgeons have devoted much time to it throughout medicine.
At the end of the 19th century, the Starling hypothesis established the following equation with the mechanisms that caused this cycle. It is still among the guiding methods, although new studies are constantly added
QF = LP × A[(PCAP - PPL) - ζD(piCAP - piPL)]
- QF, fluid motion
- LP is the filtration coefficient
- A is the pleural surface area
- ζD, reflection coefficient for protein movement over the pleura
- Hydrostatic pressure between P lung capillary bed
- oncotic pressure of the pi pleural space [2,3]
Pleural effusions are very common pathologies. It is one of the most frequently consulted diseases from chest diseases.
A significant portion of pleural effusions occurs as a complication of systemic diseases rather than a local pathology.
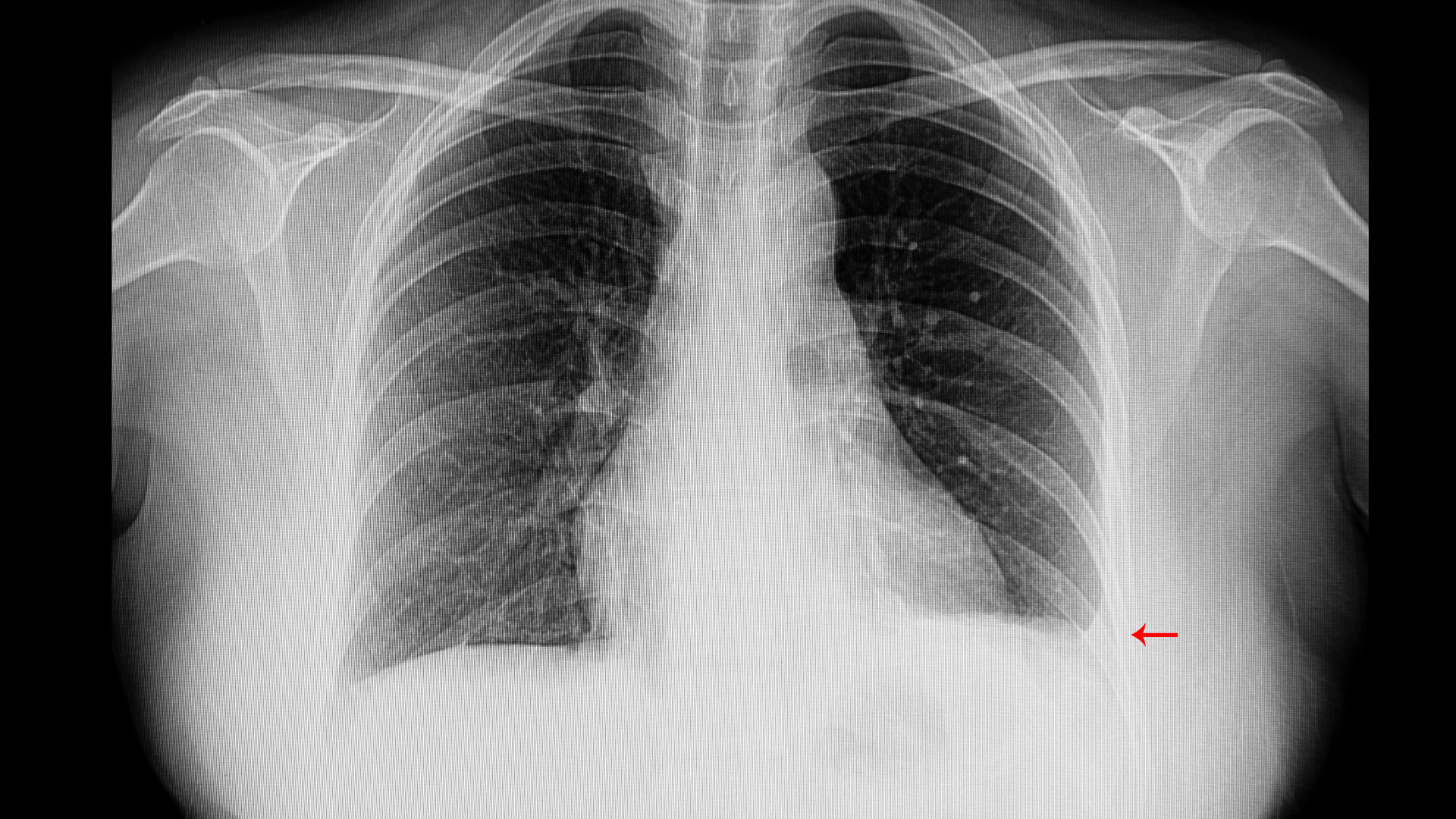
What are the Causes of Pleural Effusion?
In pleural diseases, three main pathologies come to mind:
- Pleural effusion
- Pleural thickening and plaques
- Pneumothorax
Pleural effusions are the most common and challenging to diagnose in the differential diagnosis.
The most common causes of pleural effusion are heart failure, cirrhosis, pulmonary embolism, pneumonia, tuberculosis, virus infections, and cancer of the lung or pleura.
Tuberculosis is one of the most common causes in our country. Some of the other causes are cancers, heart failure, and infections.
Congestive heart failure is the most common cause of bilateral pleural effusion in the patient.
In patients with clinical or radiological findings of heart failure, there is no need to search further for the causes of effusion; only thoracentesis is sufficient for diagnosis.
How Is Pleural Effusion Diagnosed?
The most common complaint and symptom in pleural effusions is chest pain. Two types of chest pain can occur. The pain is either stinging or blunt.
First of all, chest pain in both cases is an indication of involvement of the parietal pleura. The second most common symptom is cough.
Although the mechanism of cough formation in pleural effusion is not generally known, specialist physicians think that it may theoretically be due to inflammation of the pleura, as well as the compression caused by the effusion, the closure of the bronchi in the lung area and the stimulation of the cough reflex.
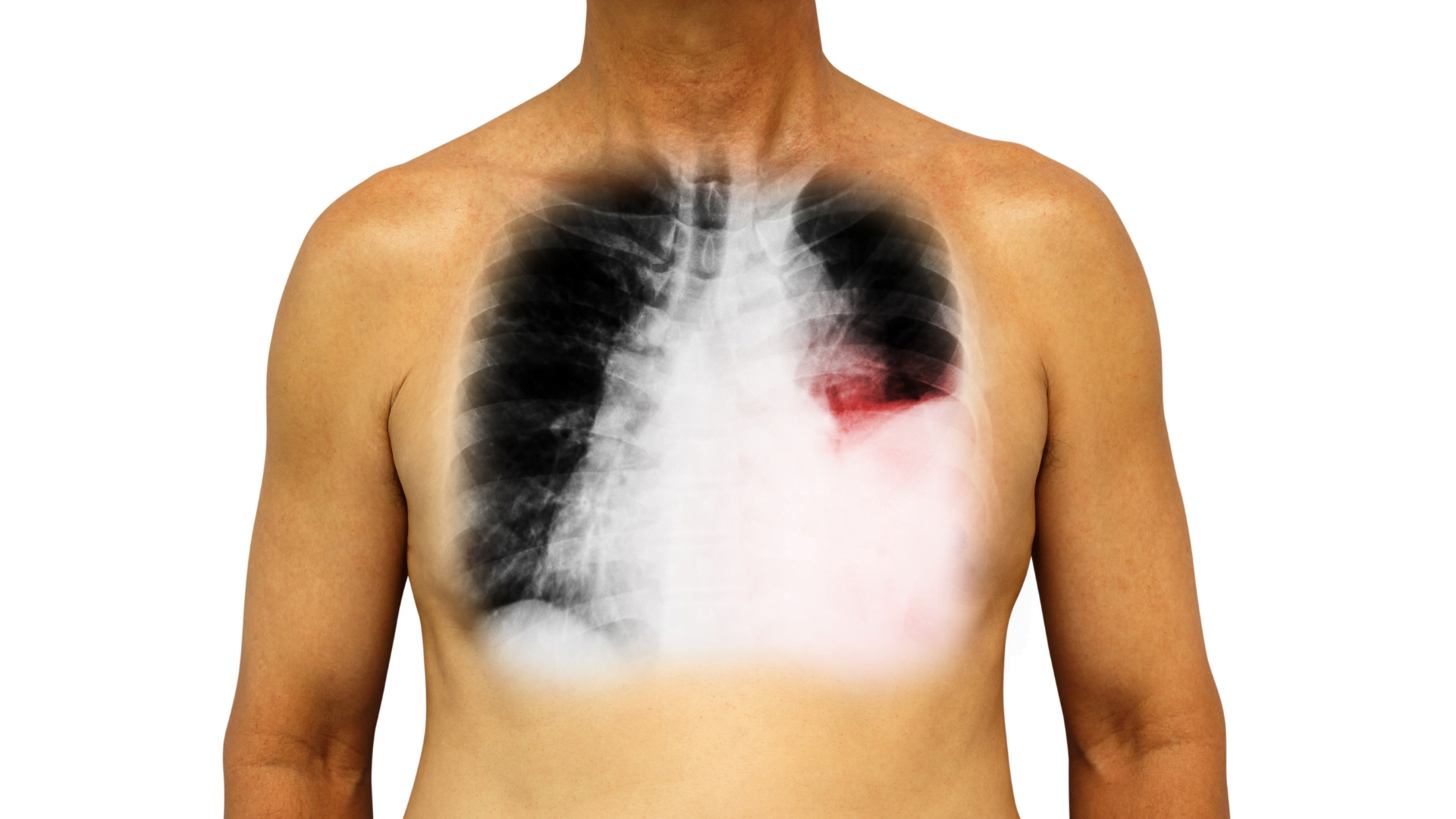
What are the Diagnostic Stages of Pleural Effusion?
Pleural effusions are also like a mirror of a person's systemic diseases. In other words, conditions belonging to all systems or organs of the patient can affect the pleura.
Thoracentesis is one of the first steps in diagnosing effusion. Thoracentesis is a procedure performed by draining at least 50 ccs with a 21 G needle from the most suitable area in the location of effusion and least complicated.
The image of the effusion is the detail that brings us one step closer to the diagnosis. Most aspirations are yellow, but this appearance is nonspecific. The appearance of the effusion is evaluated for the diagnosis.
In cases such as pneumonia, malignant neoplasm, pulmonary embolism, bloody effusion may occur. If the fluid is cloudy or milky, chylothorax, pseudo chylothorax, and empyema are suspected. Afterward, centrifugation is performed, and if there is precipitate, we can say it's empyema.
The diagnosis of pleural effusion begins with the patient's history and performing a physical examination. Analysis continues after chest X-ray and pleural fluid aspiration. A small amount of pleural fluid accumulation may be asymptomatic.
15% of pleural effusions may be asymptomatic, and other investigations such as thoracic computed tomography, pleural biopsy, thoracoscopy, and sometimes bronchoscopy are helpful if necessary.
One of the first issues to be considered in diagnosing bilateral or unilateral effusion in the patient is whether there is heart disease accompanying it. The differential diagnosis range of bilateral effusion is narrow.
It is challenging to diagnose patients with unilateral effusion. Physicians, and experts in the subject, create algorithms to facilitate the diagnosis of these patients.
What Kind of Conditions Cause Pleural Effusion?
Some medications can cause effusion, and in patients with unilateral effusion and undiagnosed patients, thoracic ultrasounds are required to investigate the presence of a septum.
This procedure, performed by experienced physicians, successfully shows the septum in the fluid and can minimize the complications that may occur while sampling the pleura and pleural fluid.
How Is Pleural Effusion Treated?
In comorbidities such as heart, liver, kidney failure, hypoalbuminemia, pulmonary embolism, and rheumatoid arthritis, transudate fluids can form bilateral pleural effusion.
The effusion develops rapidly, and the drug therapy initiates with diuretics. The treatment of pleural effusion varies depending on the patient's disease causing the effusion.
When the effusion is enormous that it causes respiratory distress and extreme shortness of breath, there are several methods to drain the fluid.
Sometimes this fluid accumulates in different body parts, gets inflamed, and creates pus.
There are some difficulties in treating pleural effusions from cancer to the lung membrane.
Life expectancy in these patients is usually short. It aims to drain the fluid and prevent fluid accumulation recurrence with adhesive treatment (pleurodesis). Although the success rate is low, it is possible to repeat the treatment.