What is Thymoma?
The thymus gland is a small organ located under the sternum in the anterior mediastinum.
The thymus is part of the immune system and is responsible for developing T lymphocytes.
Lymphocytes circulate throughout the body and fight infection. As we age, the thymus regresses, but in some people, a remnant tissue remains.
What is Thymoma / Thymic Carcinoma?
Thymoma is a slow-growing tumor that does not usually spread beyond the thymus gland. It is the most common tumor in the anterior mediastinum in adults.
Thymic carcinoma is less common but more aggressive. It is often more challenging to treat because it spreads quickly to other body parts. Both tumors typically begin in thymic epithelial cells.
Thymoma / thymic carcinoma are both rare types of cancer. There are about 400 cases (combined) per year in the United States, and about 1.5 people per million are diagnosed with thymoma/thymic carcinoma. The World Health Organization (WHO) has developed a classification system for thymoma. This system identifies six types of thymomas based on the cells that make up the tumor. The histological type and other factors determine the staging and treatment modalities.
What Are the Symptoms of Thymoma / Thymic Carcinoma?
Approximately one-third of patients are asymptomatic in thymoma/thymic carcinoma. Symptoms, if present, include cough, chest pain, shortness of breath, hoarseness, decreased appetite, and difficulty swallowing. Rarely thymoma/thymic carcinoma tumors can press on the superior vena cava (SVC) and lead to a complication called SVC syndrome.
The SVC is the primary blood vessel that brings blood from the upper body to the heart. Symptoms of SVC syndrome include swelling of the neck, chest, and face, swelling of the visible veins in the upper body, headache, and dizziness. SVC syndrome is a severe condition that requires immediate medical attention.
Some patients may present with conditions caused by the tumor itself. These include myasthenia gravis, red cell aplasia, and hypogammaglobulinemia. These are autoimmune conditions in which the body's immune system appears to attack itself.
Other autoimmune diseases are associated with thymomas, such as lupus, polymyositis, ulcerative colitis, rheumatoid arthritis, Sjogren's syndrome, sarcoidosis, and scleroderma. If you have one of these autoimmune diseases, talk to your healthcare team about screening for thymoma.
How Is Thymoma / Thymic Carcinoma Diagnosed?
Thymoma is usually diagnosed based on x-rays and images of the chest. Laboratory studies such as routine blood work are generally not used. A biopsy is rarely done for diagnosis because healthcare providers can often diagnose thymoma based on imaging such as chest X-ray, CT scan, or MRI. PET-CT shows the spread of the tumor.
Routine blood for differential diagnosis of mediastinal masses; Other tumor-specific markers such as LDH, AFP, and B-HcG are essential.
We generally prefer surgery without biopsy if a clinical and radiological thymoma is considered. Since the tumor is likely to spread if its capsule is punctured. If a biopsy is required for differential diagnosis;
- Tru-cut or fine needle biopsy (TTIAB) can be performed. We generally prefer Tru-cut biopsy because we want thick tissue for staining. It is often challenging to diagnose mediastinal masses with TTIAB/ Tru-cut biopsy.
- Mediastinotomy; In this procedure, an incision is made above the 2nd rib of the chest, and a piece of the tumor is removed. It is our most preferred method.
- Thoracoscopic biopsy (Video Assisted Biopsy (VATS); Sometimes, we prefer it if there are suspicious foci in another place other than the mediastinum.
Type A
It is called a spindle cell or medullary thymoma. The cell is a spindle-shaped or oval epithelial cell that appears quite normal. It constitutes 4-7% of all thymomas. About 17% of cases may be associated with myasthenia gravis.
Type AB Mixed Thymoma
The cells look like type A but also contain non-neoplastic lymphocytes. It constitutes 28-34% of all thymomas. About 16% of cases may be associated with myasthenia gravis.
B1 Type
Lymphocyte-rich thymoma (also called lymphocytic thymoma, predominantly cortical thymoma, organoid thymoma). The cells show many lymphocytes in the tumor, but the thymus cells appear healthy. It constitutes 9-20% of all thymomas. About 57% of cases may be associated with myasthenia gravis.
B2 Type
Cortical or polygonal cell thymoma is defined as the presence of many lymphocytes and abnormal thymus cells. It constitutes 20-36% of all thymomas. About 71% of cases may be associated with myasthenia gravis.
B3 Type
Epithelial thymoma (also known as atypical thymoma or squamoid thymoma) is a well-differentiated thymic carcinoma. The cells contain few lymphocytes and abnormal thymic cells. It constitutes 10-14% of all thymomas. About 46% of cases may be associated with myasthenia gravis.
Type C Thymic Carcinoma
Thymic epithelial tumor cells resemble carcinomas in other organs. The association between Myasthenia gravis and thymic carcinoma, which always lacks immature lymphocytes, is rare.
How Is Thymoma Staged?
Once a thymoma is found, further testing may be needed to see if the tumor has spread. The extent of tumor spread is vital in staging. The Masaoka staging system is the most widely used for staging thymoma/thymic carcinoma. Staging through this system considers the extent of disease seen by CT/MRI, the tumor spread to nearby tissues, and histological typing (cell type).
What Are The Treatments For Thymoma / Thymic Carcinoma?
Surgical tumor removal is the primary treatment for thymoma/thymic carcinoma. The first step is to determine whether the tumor can be surgically removed (resectable) depending on several factors. If the tumor has spread to nearby tissues and organs, it may not be resectable. In addition, the patient may be unable to operate because of other pre-existing medical conditions. A thymectomy, the complete removal of the thymus, is the most common surgery for treating thymic cancers. If the tumor is not completely resectable, meaning that it cannot be surgically removed, in these cases, chemotherapy or radiation may be used before surgery to reduce the tumor's size to aid in its removal. It is called surgery after neoadjuvant therapy.
- Thoracoscopic /VATS; It is the most preferred method. It is a closed method with two or three incisions. Thymoma/thymic carcinoma is resected without cutting the sternum and through small incisions. It has many advantages, including aesthetics, less pain, and early discharge.
VATS; should not be preferred in tumors with a huge diameter to prevent the tumor's spreading.


Figure 1: Videothoracoscopic and robotic thymectomy surgery positions and incisions in our clinic. Thymus and adipose tissue with poles removed thoracoscopically.
- Robotic surgery
The surgeon makes small, precise movements with his hands, wrists, and fingers and converts these movements into real-time micro-movements. A surgeon standing at the patient's bedside during the operation helps the surgeon at the console. Like our eyes, the procedure is under a 3D image with a sense of depth on the console. The operation area is enlarged 10-12 times with cameras.
By magnifying the anatomical structures in deep and narrow areas with the camera, injuries that may occur during surgery are minimized. The surgeon gives commands using the camera and other tools with the help of his hands and feet.
Thanks to the system called 'endowrist,' these tooltips can rotate 540 degrees around their axis and imitate the wrist movements of the human hand. In robotic surgery, the possible hand tremor of the surgeon during the operation is not transmitted to the instruments in any way.

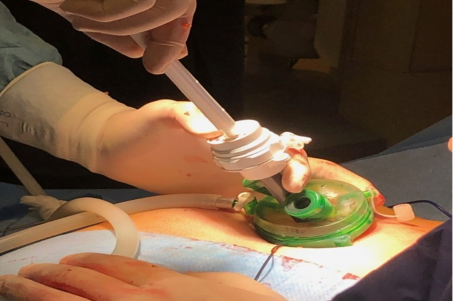
Figure 2. Subxiphoid Robotic Thymectomy
- Median Sternotomy: Median sternotomy should be the standard approach in locally advanced cases, especially if large vessels are involved, superior vena cava invasion, and the tumor diameter is huge.
- Thoracotomy: Sometimes, if the tumor's location is risky, we prefer to perform a thoracotomy.
Since Myasthenia Gravis sometimes accompanies thymomas, it is essential not to cut the phrenic nerves. If cut, he may experience severe respiratory distress.
Radiation Therapy
Thymomas are susceptible to radiation therapy treatment.
Radiation is not needed for noninvasive thymoma tumors that have been completely removed. Radiation is for stage III or IV tumors after complete or partial surgical removal of cancer. Whether radiation is required after the complete surgical removal of stage II tumors is unclear and often depends on the patient and the characteristics of their tumors. Radiation is usually recommended to reduce the chance of tumor recurrence. Radiation can be used in any stage of thymoma where it is technically impossible to perform safe and complete surgery.
Chemotherapy
The use of chemotherapy for advanced tumors has increased. Some thymic cancers are treated with targeted therapies that focus on specific tumor mutations or proteins found in that tumor.
Follow-up and Care of Thymoma Disease
After treatment for a thymoma or thymic carcinoma is completed, your doctor and healthcare team will monitor you closely. There is no widely accepted follow-up program for survivors. Still, your team will follow up for the first three months after treatment and every six months after that to monitor for late treatment-related side effects and possible relapse. You may need a thoracic CT scan every six months for 1-2 years after treatment.
Fear of relapse, relationship difficulties, the financial impact of cancer treatment, employment issues, and coping strategies are all emotional and practical problems experienced by survivors. Your healthcare team can identify resources for supporting and managing these practical and emotional challenges during and after cancer.
Frequently Asked Questions About Thymoma
Many people have question marks about thymoma disease. We have compiled some of the questions about this disease for you below; here are the questions that most people wonder:
Since the thymoma can be easily removed, most are curable. Especially in Stage 1, since the tumor is in a capsule, it can be easily removed, and its survival is excellent. There is a capsular invasion in stage 2, survival is still better, and no additional treatment is necessary after surgery. Since there is metastasis to surrounding tissues in stage 3, survival is better when CT/RT comes after the surgery. We do not operate the patients with distant metastasis in stage 4; they receive oncological treatment. But in some selected cases, Stage 4a, If the thymoma has spread to the pleura or pericardium, multimodality treatment is applied. We do not prefer surgery in Stage 4b; systemic chemotherapy, radiotherapy, and immunotherapy are suitable.
Thymoma is cancer that usually spreads locally. Since it has a capsule, its survival is good after surgery.
Thymomas are slow-growing tumors, and their prognosis is excellent when discovered early. Thymoma has a capsule, which prevents its spread. Surgical removal is the primary treatment.
The cause of the thymoma is unknown. Risk factors are not apparent. It affects men and women equally and mainly occurs in people aged 50-60. People with thymoma may have other diseases of the immune system. Myasthenia gravis, an autoimmune condition that causes muscle weakness, is a frequently thymoma-associated syndrome and may be present in approximately 30% of thymoma patients. Conversely, only 10-15% of patients diagnosed with myasthenia gravis develop thymoma, as myasthenia gravis is more common than thymoma.
There is no screening test for thymoma/thymic carcinoma. Almost half of those with thymoma/thymic carcinoma have no symptoms when the tumor is diagnosed. Thymoma is often diagnosed incidentally when an X-ray or CT scan is done for another reason.
Thymoma usually does not spread beyond the chest. Thymic carcinoma is more likely to spread throughout the chest and other parts of the body (distant areas). If thymus cancer spreads, it most commonly spreads to nearby fatty tissue.
We generally prefer surgery without biopsy if a clinical and radiological thymoma is considered. If a biopsy is required for differential diagnosis;
We perform Tru-cut or fine needle biopsy (TTIAB). We generally prefer Tru-cut biopsy because we want thick tissue. It is often challenging to diagnose mediastinal masses with TTIAB/ Tru-cut biopsy.
Mediastinotomy; In this procedure, an incision is made above the 2nd rib of the chest, and a piece of the tumor is removed. It is our most preferred method.
We prefer Robotic Surgery or VATS (Thoracoscopy) in thymoma Stages 1-2. Instead of cutting out the sternum, it is a very comfortable procedure to enter through 2 or 3 incisions with Robotic surgery or VATS and remove the tumor. Robotic Surgery or VATS; should not be preferred in tumors with a huge diameter.
It means that the thymoma has spread to the pleura or pericardium, but there is no metastasis to other organs. Multimodality treatment is applied to Stage 4a cases. In some patients, chemotherapy and sometimes radiotherapy is administered first. After the multimodality treatment, the mass and the entire parietal pleura and pericardium are surgically resected. But we do not prefer surgery in Stage 4b; systemic therapy, chemotherapy, radiotherapy, and immunotherapy are suitable for these cases.

